Patients and relatives
CGFL is a hospital and research center specialized in cancerology.
Together, let’s overcome cancer.
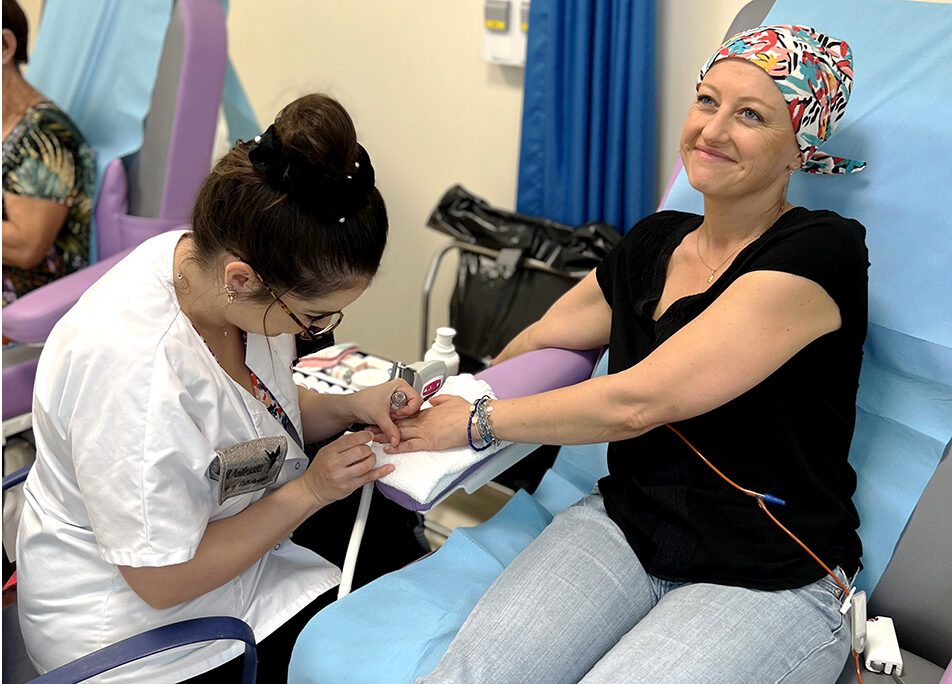

CGFL is a hospital and research center specialized in cancerology.
The CGFL is one of the 18 Cancer Centers (CC) grouped under the Unicancer Federation.
All CLCCs operate 100% publicly and play a major role in healthcare provision and research. Since their creation (by order of General de Gaulle on October 1, 1945), they have contributed to the public hospital service, with a constant commitment to improving the quality and accessibility of care.
Our establishment offers a personalized care model to each patient, both in terms of care and in terms of monitoring and support.
The CGFL’s healthcare range covers all cancer treatments: surgery, radiotherapy, brachytherapy and chemotherapy.
Each patient benefits from tailored treatments, thanks to the in-depth, multidisciplinary expertise of the oncology medical teams.
Surgery
Surgery is a standard treatment in the management of cancer. It aims to remove the tumor as well as any nearby tissues or lymph nodes that may be affected. In certain cases—such as after the removal of a breast, skin (particularly sarcomas), or digestive tumor—reconstructive surgery may be considered.
When a mastectomy is necessary, whenever possible, our team offers immediate breast reconstruction. The CGFL offers a full range of breast reconstruction techniques, including flaps with microsurgery.
[ AT CGFL: The surgery department treats most adult cancers. Operations are performed by a
The CGFL has acquired a DA VINCI XI surgical robot
At the cutting edge of innovation, the Da Vinci Xi surgical robot installed at the CGFL offers high-precision movements and integrates a high-definition imaging system. In addition, the surgical console can be connected to an ultrasound system, whose images are projected directly onto the control screen to guide the surgeon throughout the procedure.
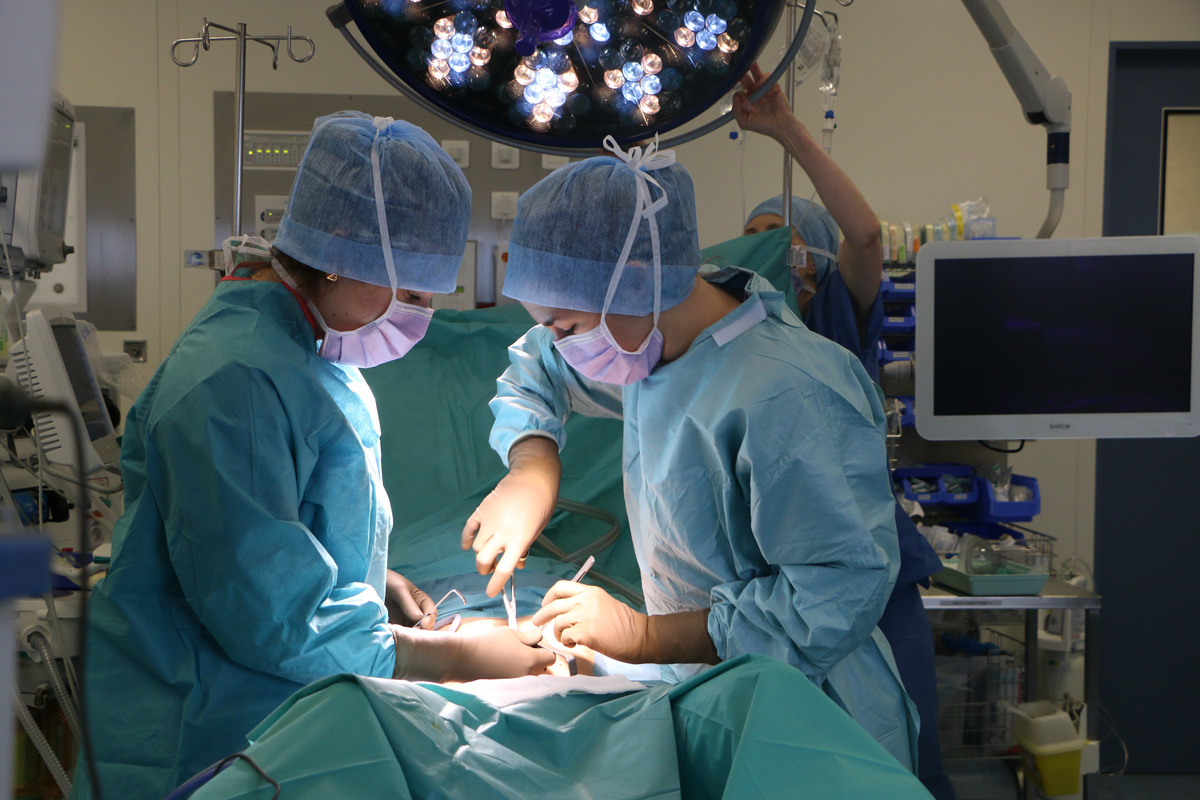
Chemotherapy
Chemotherapy refers to drug treatments that destroy cancer cells or prevent them from multiplying. It can be administered intravenously, orally, intramuscularly, and more rarely directly into the tumor. Chemotherapy can be adjuvant, concomitant, or combined with other therapies.
At the CGFL, chemotherapy is prepared within our establishment and can be administered in the Day Hospital or in conventional hospitalization.
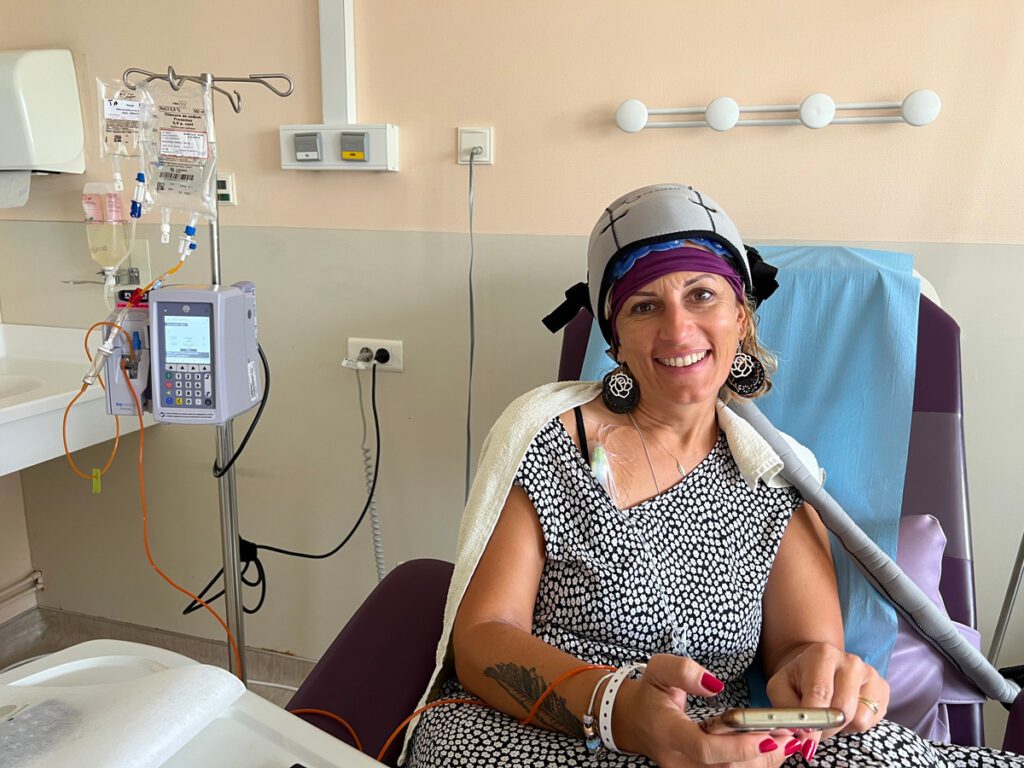
Radiotherapy
Radiotherapy is a locoregional treatment that uses ionizing radiation to destroy cancer cells while preserving healthy tissue and surrounding organs.
It can be prescribed for curative or palliative purposes and can be given alone or in combination with other treatments (e.g.: surgery, chemotherapy, hormone therapy, etc.).
There are two types of radiotherapy depending on the location of the radiation source in relation to the patient (internal or external)
- External radiotherapy
The radiation is produced by a machine called “a linear particle accelerator”. It is emitted in the form of beams directed towards the area to be treated.
During treatment, the patient lies motionless on a table, and the machine moves around him.
The size and shape of the beams are precisely adjusted to deliver the dose to the tumor while limiting irradiation of surrounding tissues.
- internal radiotherapy or brachytherapy.
Radiation comes from radioactive sources that are placed in contact with tissues or implanted inside the patient. High doses of radiation are delivered as close as possible to the tumor.
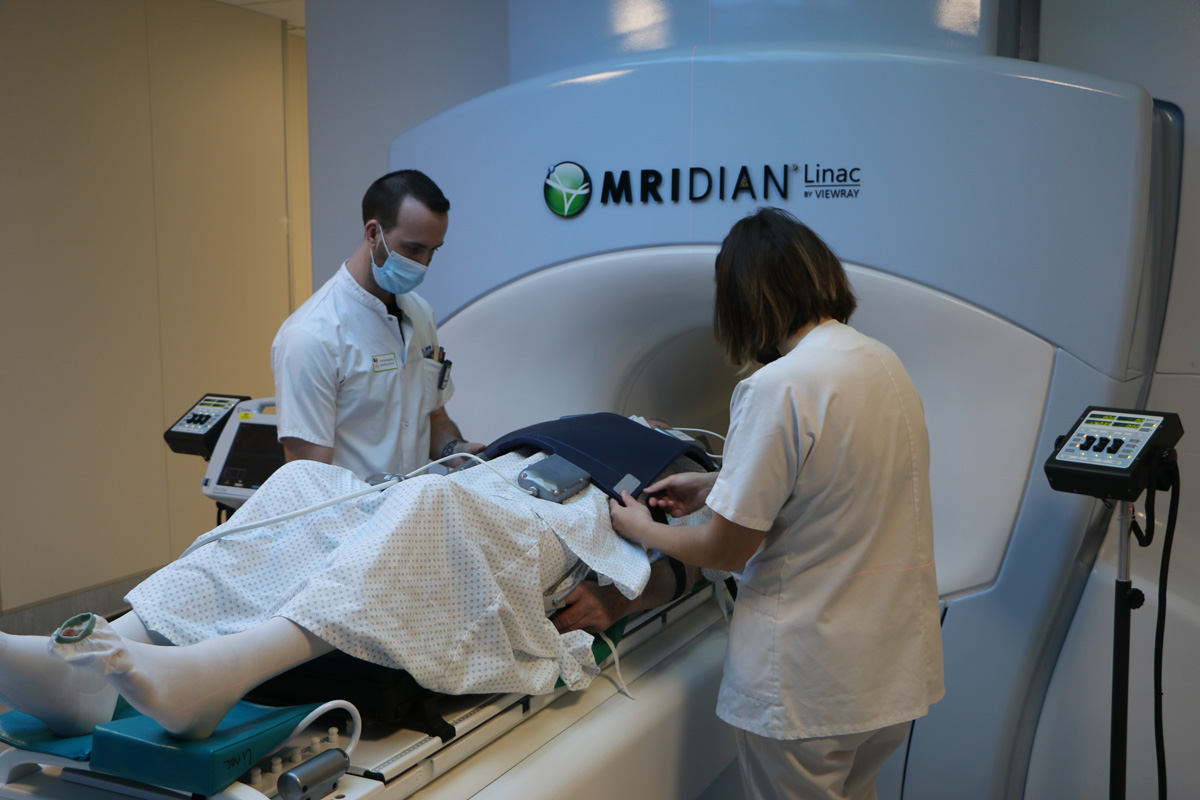
The CGFL is one of the first centers in France to be equipped with a Linac MRI
Coupled with a magnetic resonance imaging system, this radiotherapy device revolutionizes patient care by allowing more targeted, more precise irradiation, while ensuring maximum protection of neighboring healthy organs. Throughout the treatment, this non-irradiating imaging allows for permanent visual monitoring of the tumor and real-time monitoring. It is also able to take into account, at each session, anatomical changes in the tumor or nearby organs, in order to be able to offer the patient “personalized adaptive” radiotherapy. This innovative technology is particularly suited to mobile or very small tumors.

The CGFL has acquired 4 photobiomodulation machines
Photobiomodulation (PBM) is a technique that uses red or near-infrared light from different light sources to provoke a response at the cellular level.
It is used for its analgesic, anti-inflammatory and tissue healing properties.
It is non-invasive, painless and has no heat effect on the skin.
Photobiomodulation can be used to mitigate the effects of chemotherapy or the consequences of radiotherapy. It can also be offered by the institution’s pain management service, which has one of the four devices currently available at the CGFL.
At the CGFL, the radiotherapy technical platform is made up of :
1 dedicated scanner: Siemens SOMATOM Go.Sim
5 accelerators: 1 Varian Truebeam®, 1 Varian Novalis®, 2 Varian Halcyon®, 1 IRM Linac
1 VisionRT® Surface Repositioning System
2 brachytherapy source projectors
2 photobiomodulation devices: Caremin 650 and ATP38
Vectorized Internal Radiotherapy at CGFL
A breakthrough therapeutic innovation for the treatment of certain metastatic cancers, Vectorized Internal Radiotherapy consists of administering to patients small molecules carrying a radioactive atom, which will recognize and attach to a target expressed or overexpressed by tumor cells.
Thus, the radioactivity delivered directly to the tumor cells will cause damage to their DNA, stopping the progression of the disease.
These treatments are administered under the responsibility of nuclear medicine physicians, in close collaboration with medical oncologists.

Immunotherapy
Immunotherapy relies on harnessing the immune system’s defense mechanisms to attack and eliminate cancer cells. Over the decades, several methods have been explored, with a particularly promising approach recently emerging: administering drugs designed to alter the behavior of immune cells, breaking their tolerance toward tumor cells and thus activating their ability to destroy them.
At the CGFL, immunotherapy has now become a key part of the center’s two major missions: research and care.
In research, the CGFL teams are conducting several studies on the role of the immune system and resistance mechanisms (particularly in digestive, skin, and lung cancers) as well as on circulating DNA or circulating cells. This work aims to better describe the anti-tumor immune response.
On the care side, several CGFL patients have already benefited from this innovative treatment as part of therapeutic trials.
These phase I, II, or III trials are conducted within the Clinical Research Center.
Hormone therapy
The multiplication of certain types of malignant cells is dependent on hormones. These include breast and prostate cancers.
Prostate cancer and hormone therapy: It slows the growth and spread of prostate cancer cells by blocking their receptors or altering hormone levels in the body.
Breast cancer and hormone therapy
In premenopausal women:
- Antiestrogens are most often proposed as the first treatment for a duration of 5 years
- LH-RH agonists can be considered on a case-by-case basis, over a period of 3 to 5 years.
In menopausal women:
- Aromatase inhibitors are most often proposed as the first treatment for a duration of 5 years or for 2 years, followed by treatment with tamoxifen (for a total of 5 years of hormonal therapy).
- Antiestrogens may be offered for 2 to 3 years, followed by an aromatase inhibitor (for a total of 5 years of hormone therapy) or, alone, for 5 years.
Interventional radiology
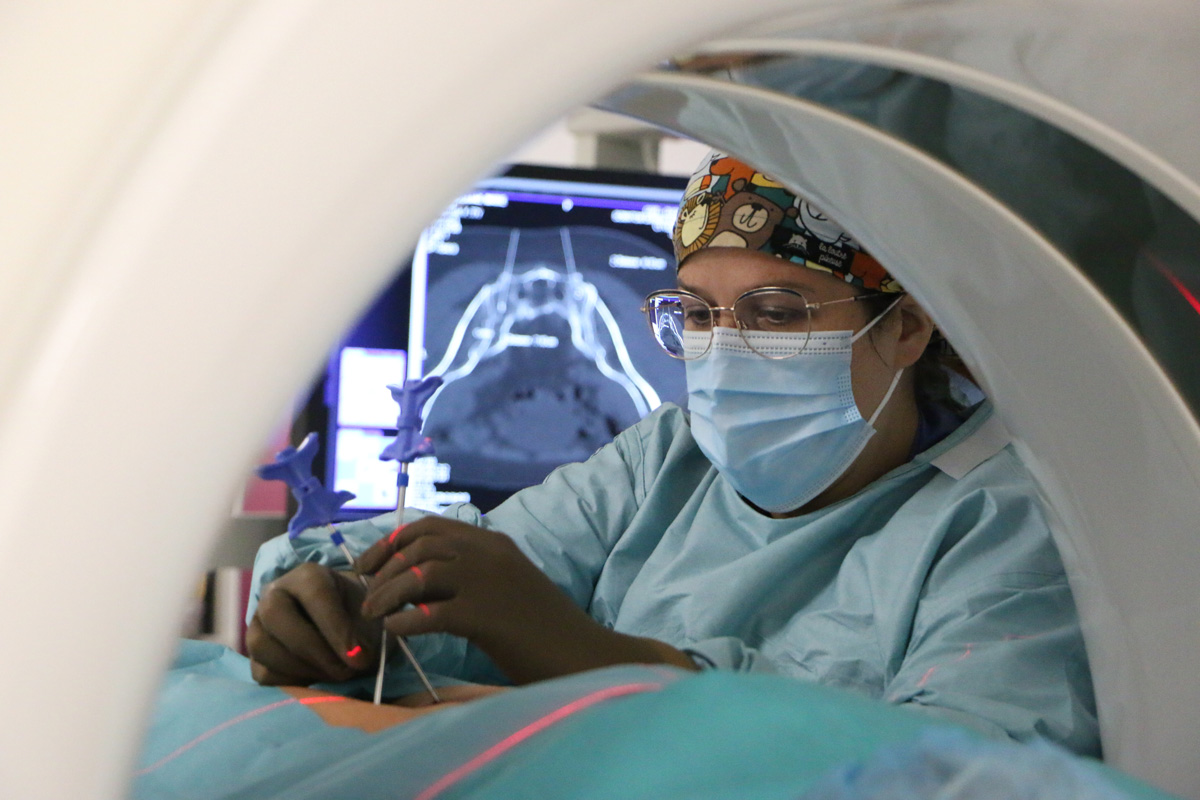
Interventional radiology is a diagnostic and therapeutic technique known as “minimally invasive” which allows deep tumors to be reached using natural pathways (such as the urinary or digestive system), the vascular network (arteries or veins), or by taking a short and safe route through an organ.
These interventions are guided by imaging techniques (scanner, ultrasound, endoscopy), allowing the interior of the body to be visualized without resorting to open surgery.
Vectorized Internal Radiotherapy at CGFL
The CGFL has acquired 4 photobiomodulation machines.
Photobiomodulation (PBM) is a technique that uses red or near-infrared light from different light sources to provoke a response at the cellular level.
It is used for its analgesic, anti-inflammatory and tissue healing properties.
It is non-invasive, painless and has no heat effect on the skin.
Photobiomodulation can be used to mitigate the effects of chemotherapy or the consequences of radiotherapy. It can also be offered by the institution’s pain management service, which has one of the four devices currently available at the CGFL.