Our supportive care
They aim to improve the quality of life of sick people.
Together, let’s overcome cancer.
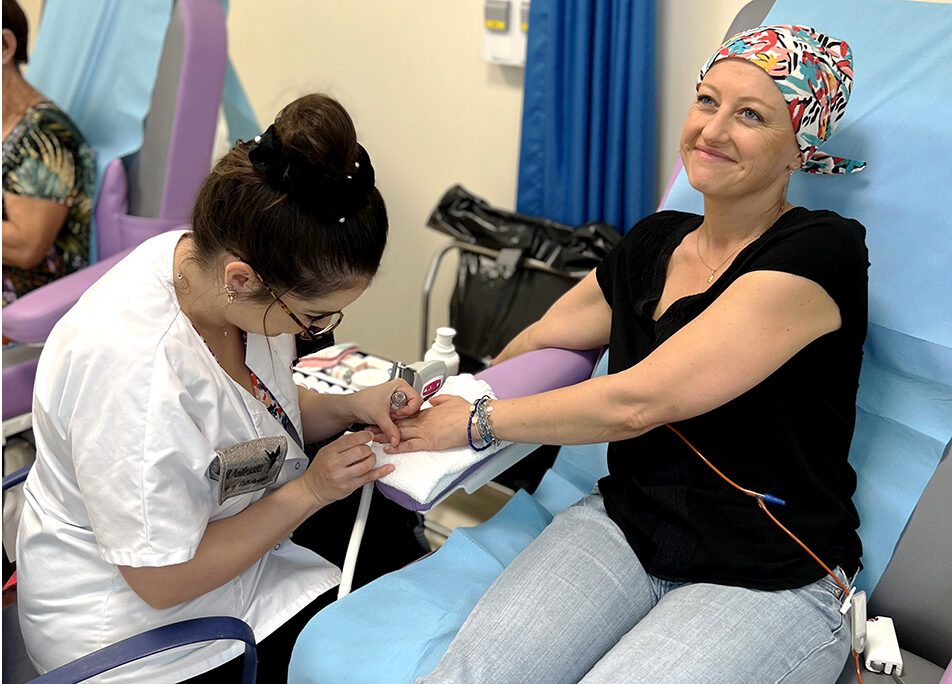

Supportive care at CGFL
Supportive oncological care includes: “all the care and support necessary for sick people throughout the illness in conjunction with specific onco-hemato treatments, where available” (Circular No. DHOS/SDO/2005/101 of February 22, 2005 relating to the organization of cancer care).
The National Cancer Institute (Inca) defines the basket of supportive care with 4 “basic” care (pain management, dietetics and nutrition, psychological, social, family and professional) and 5 complementary supportive care (physical activity, psychological support for relatives and carers, preservation of fertility, management of sexual disorders, advice on healthy lifestyle) and 2 specific analgesia techniques (hypno analgesia and intrathecal analgesia).
Supportive care not only helps improve the quality of life but also the lifespan of patients. It helps prevent or limit certain side effects of cancer treatments and thus limits their interruptions, whether temporary or permanent.
THE DT2S
The Cross-Department of Supportive Care (DT2S) was created in 2018. Gradually strengthened, it allows patients and their loved ones to benefit from supportive care adapted to their situation. In 2024, the CGFL was labeled by the Multinational Association of Supportive Care in Cancer as a “center of excellence in supportive oncological care” (A MASCC-Designated Center of Excellence in Supportive Care). The CGFL is one of only four French centers thus recognized by the MASCC.
Day Hospital Supportive Care
Patients admitted to the Day Hospital supportive care unit come from home, post-acute care facilities, or outlying hospitals. The supportive care unit’s system allows for a comprehensive assessment of their needs in a shorter timeframe.
All supportive care specialists who work with patients are organized to provide care in their rooms for a half-day. This multi-professional approach is provided without the patient needing to travel.
The social work team’s mission is to advise, guide, and support patients and their loved ones in dealing with the social consequences of the illness. Social workers assist patients in their social processes to resolve any difficulties they may encounter.
Patients can call on social services at any time during their care journey.
Its fields of action include:
- Administrative procedures and access to health-related rights,
- assistance with returning home after hospitalization,
- maintaining and returning to employment after illness.
Discover the service’s Social Tutorials.
Psychologists support patients and their loved ones at any stage of their care, at their request or at the suggestion of healthcare professionals. Depending on needs, psychological support will be offered on an ad hoc basis or as part of a follow-up program.
Specific support is offered to young patients aged 15 to 30, through a systematic meeting with the psychologist and the social worker, in conjunction with the various support care professionals.
The neuropsychologist works with patients with cognitive complaints, at their request or at the suggestion of health professionals, by offering assessments of cognitive disorders in order to direct them to the appropriate community professionals (neuropsychologist, speech therapist, etc.).
The use of a wide variety of techniques and treatments allows for the adaptation and personalization of patient care in oncology or post-surgical settings (pain relief, bed-rest prevention, maintaining or recovering motor and/or respiratory abilities, etc.).
Assessment activities allow for optimal patient guidance and advice, particularly regarding their hospital discharge (equipment, fall prevention, physical activity, etc.).
The physiotherapists and the Adapted Physical Activity instructor coordinate their activities with the common goal of optimal care for hospitalized patients.
The EAPA offers muscle strengthening exercises, retraining for exercise, and sound advice on good practice…
This adapted physical activity can have benefits in the context of surgery in order to prepare the body to best withstand the intervention, but also post-operatively to optimize recovery. In the context of treatments (chemotherapy, radiotherapy, etc.), it helps combat their side effects and in particular reduce fatigue. Monitoring can also be done remotely thanks to the use of a digital platform that allows you to continue adapted physical activity outside of the hospital.
Nutritional deficiency is very common in cancer, and manifests itself primarily through weight loss. The dietetics team, working with the medical and catering teams, provides the necessary support to maintain a balanced diet during treatment.
Dietitians offer practical ideas for successfully developing appetite and increasing daily calorie intake. Sometimes, nutritional supplements are necessary. In this case, a doctor or dietitian will prescribe them.
In each situation, measures can be taken to maintain the pleasure of eating according to one’s tastes and habits. These measures are adapted to the constraints linked to the state of health and treatments.
The socio-hairdresser provides support to patients before, during and after hair loss or any other hair changes that appear following treatment.
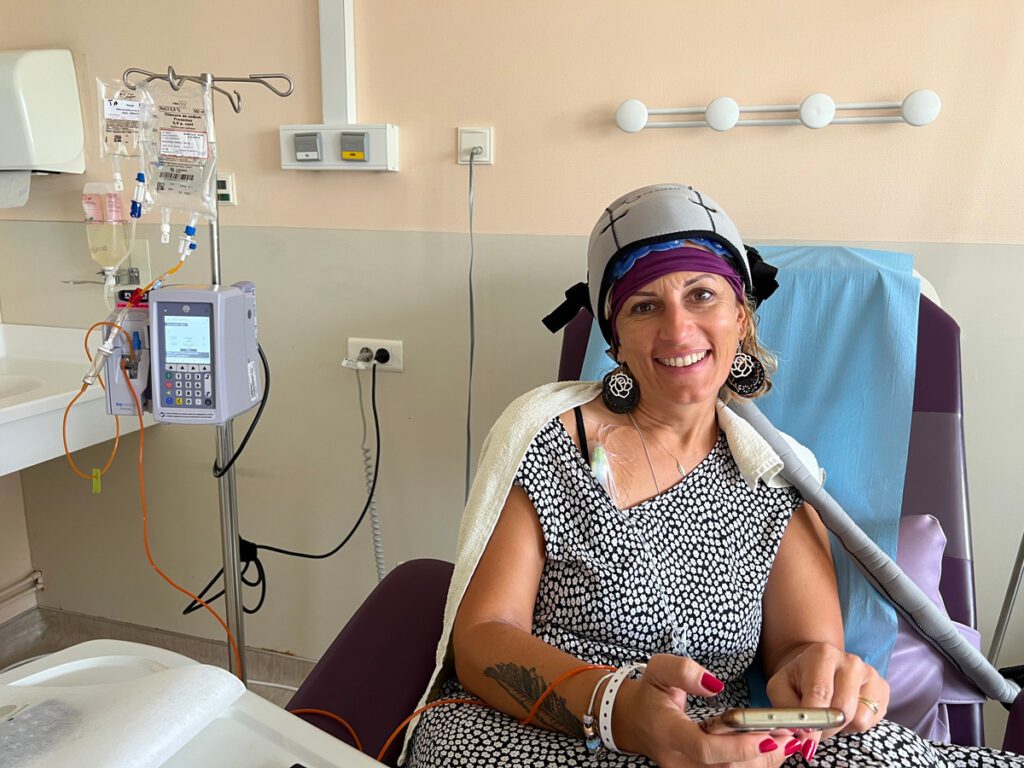
The socio-hairdresser provides advice on preventing treatment-related hair loss and offers tailored treatments: shampooing, cutting, massaging, and moisturizing the scalp. She is available to explain alternatives related to hair loss and refer patients to hair prosthetists. Cooling caps are available in the day hospital, depending on the type of treatment, to limit hair loss. These special moments contribute to the enhancement of self-esteem in order to promote identity repair.
Completely free, socio-hairdressing and socio-aesthetic treatments are provided in individual sessions or through group workshops (workshop on tying a turban, a scarf / hair prosthesis workshop / scalp massage workshop.
A professional beautician is available to provide free care. In a specially designed treatment room, in a room, or even in a day hospital during chemotherapy sessions, her treatments are personalized to best support patients throughout their treatment. She helps patients better cope with adverse skin effects.
Its fields of action include:
- Provide skin care advice and products to use during treatments.
- Promote identity repair and enhance self-image
- Offer treatments such as nail care and makeup, as well as hand and foot care.
Socio-hairdressing and socio-aesthetic treatments are provided in individual sessions or through group workshops (workshop on tying a turban, a scarf / hair prosthesis workshop / scalp massage workshop.
Our care for more specific support
The Mobile Palliative Care Team (MPCT) is a multi-professional team specifically trained in palliative care and support. The MPCT travels throughout the facility at the request of the patient, relatives, or healthcare professionals. Consultations or supportive care day hospitals can also be organized.
The EMSP provides comprehensive support and assessment for each situation and makes appropriate recommendations. It helps manage symptoms and recommends the prescription of certain treatments. It also coordinates with various external teams to enable patients or their families to return home or remain at home when they so wish.
The role of the wound healing nurse is to optimize the care of oncology patients who also have wounds by assisting the various healthcare providers within and outside the institution. Their training allows them to understand, in collaboration with other healthcare professionals, all kinds of wounds, whether acute, chronic or resulting from cancer treatments (surgery, radiotherapy, oncology, etc.). They promote the link between the hospital and the liberal professions in order to ensure the safe return home of patients and remain available for outpatient consultations for the follow-up of certain wounds.
The stoma therapist nurse sees any patient whose care requires the placement of a stoma (or diversion), whether it is of digestive, urinary or ENT origin, including refeeding stomas. He/she sometimes participates in the management of certain complications such as fistulas or continence problems. He/she accompanies the patient before the intervention, provides aftercare and educates him/her until independence so that he/she can regain a satisfactory personal, family, professional and social life. He/she is active in numerous care pathways within and outside the establishment and remains available for outpatient consultations.
Cancer treatments can negatively impact sexuality and affect quality of life, which is why follow-up with a sexologist is part of supportive care. Consultations can be conducted before or during treatment, in coordination with the entire medical team or at the patient’s request.
A midwife is present at the facility and leads meetings between women on the topic of sexuality, a subject that can sometimes be difficult for patients to discuss. These workshops allow patients to discuss intimate topics in complete confidence with trained healthcare professionals.
More information about the sexologist who consults at the CGFL.

The management of CGFL lymphedema is carried out by a multi-professional team: a vascular doctor, physiotherapists, nurses, dieticians, orthotists and occasionally other professionals from medical or paramedical specialties and support care (psychologists, social workers, etc.).
These professionals meet patients individually, in consultation, but also through sessions shared with other patients also affected by lymphedema. The goal of this care is to establish an indication for treatment, to implement this treatment at the Center and to ensure its follow-up by a local physiotherapist, in order to help each person live better with lymphedema.
A multi-professional care team trained in addiction medicine is available to patients and CGFL teams. Tobacco and addiction specialists, addiction nurses, and paramedical professionals working in the care teams are available to support patients in their efforts to reduce and/or stop using tobacco, alcohol, or other substances.
This team can intervene in consultations but also after hospitalizations, to compensate for a potential state of withdrawal due to involuntary and sudden withdrawal.
Stopping or reducing tobacco and alcohol consumption has a real impact on the good tolerance and effectiveness of treatments and also prevents the risk of relapse.
PBM is a treatment technique using light energy in the red and infrared range, which is known for its anti-inflammatory and healing properties. PBM is used in radiotherapy, oncology, and pain management to prevent and treat side effects such as mucositis, radiodermatitis, hand-foot syndrome, and neuropathic pain. PBM has virtually no side effects. It can be used in conjunction with other treatments.
The announcement of a serious illness is always a traumatic event for the patient. The announcement system aims to allow the patient to benefit from the best possible conditions of information, listening and support.
The announcement medical consultation presents the therapeutic proposal defined during the multidisciplinary consultation meeting. Following this medical consultation, a period of paramedical support is offered to the patient. The caregiver listens to the patient in order to understand their level of information and their concerns. They reformulate what was said during the medical consultation, re-explain and complete the information received. They direct the patient to the various support treatments and competent professionals within the establishment or in the community.

Meeting and Information Space
To accompany you
The Meeting and Information Space is a great place to find a friendly welcome, a presence, a listening ear, and to take the time to chat or simply take a break for a few moments. Numerous thematic workshops, conferences, and activities are also organized within this convivial space.

Patricia Lecerf
Health companion.
Find her on Mondays, Tuesdays, Thursdays, Fridays from 1:30 p.m. to 5 p.m. and Wednesdays from 9 a.m. to 12:30 p.m.
She can also be reached at:

Céline Bouttemy
Partner Patient.
Find her to discuss “a shared experience”, daily life with the illness, treatments, more personal questions (telling children, loved ones, managing side effects, etc.) or to redirect you to health professionals, support care or others.
Find her every Tuesday and Thursday from 9 a.m. to 12 p.m. and from 1 p.m. to 5 p.m.
Supportive care at CGFL
This is a complementary support service offered free of charge to patients and their loved ones. Supportive care aims to improve the quality of life of those affected. It is provided at all stages of care: from the moment the diagnosis is announced, during treatment, and even after the cancer has ended if there are any after-effects. It offers all the necessary care and support to those affected, in addition to specific treatments (surgery, chemotherapy, and radiotherapy).